Our Studies
VICS includes unique cohorts of extremely preterm (EP, <28 weeks’ gestation) or extremely low birthweight (ELBW, <1000 g birthweight) born across all the tertiary hospitals in Victoria. These EP/ELBW babies, along with a group of term-born infants, have been recurited since birth and seen for follow-up across childhood into adulthood.
A summary of the follow-up and measures collected for each of the VICS cohorts:

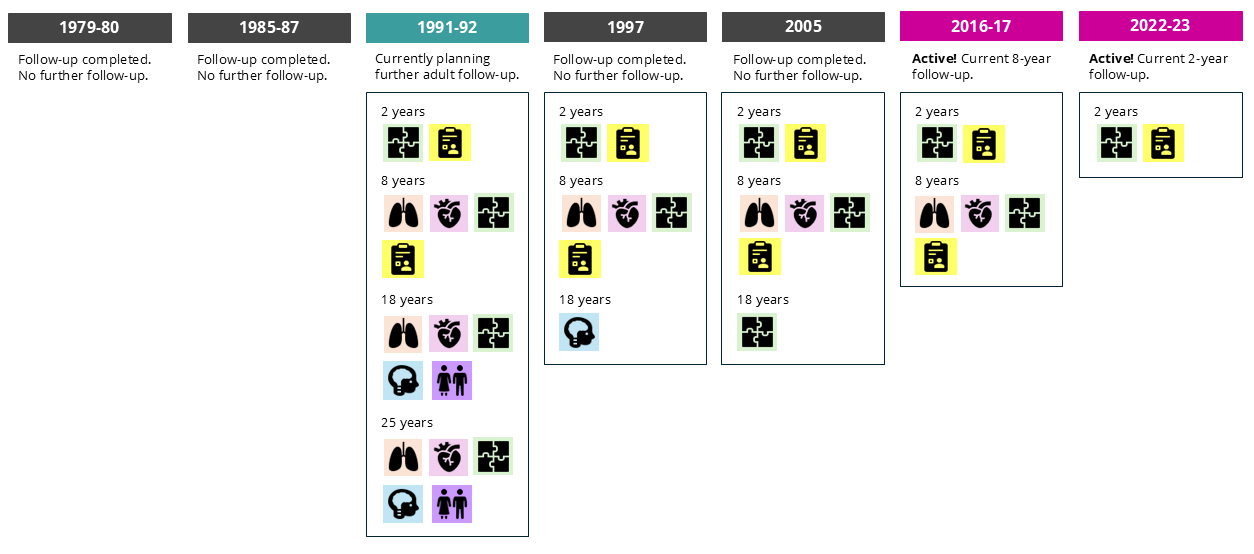
Information about the VICS cohorts
VICS 2022-23
The VICS 2022-23 cohort includes 188 infants born EP/ELBW in Victoria between 1st July 2022 and June 30, 2023. To enable meaningful comparisons, the study also includes 192 term-born infants.
Participants were recruited from Victoria’s five tertiary hospitals:
- Royal Women’s Hospital
- Monash Children’s Hospital
- Mercy Hospital for Women
- Joan Kirner Women and Children’s Hospital
- Royal Children’s Hospital
Additional recruitment occurred at Frances Perry House and Jessie McPherson Private Hospital.
Assessments: All families enrolled in the 2022-2023 VICS cohort will be invited to attend comprehensive developmental assessments at participating study locations when their child is around 2-years of age. Each child will be evaluated by a developmental paediatrician and allied health professional, who will assess growth, health status, and general developmental progress. We will also collect information on parental mental health and quality of life.
Progress: We are currently completing the 2-year follow-up assessments with this cohort and are expected to finish this phase by early 2026.
Impact: The VICS 2022-23 cohort will provide critical insights into how recent healthcare developments have influenced outcomes for premature infants and their families, in particular the impact of updated clinical guidelines recommending active neonatal care for infants born as early as 22 weeks gestation and the effects of the COVID-19 pandemic on premature birth outcomes and family experiences.
Future Directions: With continued funding support, the research team aims to maintain long-term follow-up of this cohort throughout their school years and into adulthood, providing valuable longitudinal data on the trajectory of extremely preterm birth outcomes.
VICS 2016-17
The VICS 2016-17 cohort includes 238 infants EP/ELBW infants born in Victoria between 1st April 2016 and 31st March 2017, and 225 term-born infants. Participants were recruited from Victoria’s the four neonatal hospitals at the time:
- Royal Women’s Hospital
- Monash Children’s Hospital
- Mercy Hospital for Women
- Royal Children’s Hospital
Additional recruitment occurred at Frances Perry House.
Assessments: Children in this cohort completed comprehensive developmental and medical assessments at 2 years of age. In 2024, we began an 8-year-old follow-up with this cohort which included assessments of the children’s cognitive skills, motor development, lung function, and parent mental health.
Impact: The VICS 2016-17 cohort has provided important information on the impact on contemporary medical care, and whether changes in clinical practices (since the 90’s and beyond) have had long-term influences on health and life outcomes for premature infants and their families.
Progress: We are currently completing the 8-year follow-up assessments, with data collection expected to be complete by mid-2026.
Future Directions: With continued funding support, the research team aims to maintain long-term follow-up of this cohort throughout their secondary years and into adulthood, providing valuable longitudinal data on infants born in this era.
VICS 2005
- Royal Women’s Hospital
- Monash Children’s Hospital
- Mercy Hospital for Women
Assessments: Children in this cohort completed comprehensive developmental and medical assessments at 2 years of age. In 2013-2014, we conducted 8-year follow-up assessments with this cohort, examining neurodevelopment, lung function, and cardiovascular health.
Progress: Follow-up for this cohort has finished. There is currently no active follow-up for the 2005 cohort. However, we may wish to reassess them in adulthood, depending on what we find with other cohorts in adulthood, and on obtaining funding.
VICS 1997
- Royal Women’s Hospital
- Monash Children’s Hospital
- Mercy Hospital for Women
Assessments: Children in this cohort completed comprehensive developmental and medical assessments at 2 years of age. In 2005-2006, we conducted 8-year follow-up assessments with this cohort, examining neurodevelopment, lung function, and cardiovascular health.
Progress: Follow-up for this cohort has finished. There is currently no active follow-up with the 1997 cohort. However, we may wish to reassess them in adulthood, depending on what we find with other cohorts in adulthood, and on obtaining funding.
VICS 1991-92
The VICS 1991-92 cohort includes 291 EP/ELBW infants born in Victoria between 1 January 1991 and 31 December 1992, and 231 term-born infants.
Participants were recruited from Victoria’s three tertiary hospitals at the time:
- Royal Women’s Hospital
- Monash Children’s Hospital
- Mercy Hospital for Women
Assessments: Children in this cohort completed comprehensive developmental and medical assessments at 2 years of age. In 1996-1997, we conducted 5-year follow-up assessments with this cohort, examining neurodevelopment and school readiness. In 1999-2000, we conducted 8-year follow-up assessments, examining neurodevelopment, lung function, and cardiovascular health. This cohort was then followed up at 18 years and again at 25 years of age to examine physical, neurodevelopmental and mental health, as well as transition into adult life.
Progress: The team are currently planning the next follow-up, into their mid-30s.
Impact: The introduction of exogenous surfactant to treat respiratory distress syndrome in the early 1990s was pivotal in newborn intensive care. The VICS 1991-92 cohort has provided important insights into survival rates and outcomes in babies born after the introduction of surfactant.
Future Directions: We are currently seeking funding to follow this cohort into middle adulthood.
VICS 1985-87
Impact: Research results from this cohort have helped track the trajectory of change in outcomes as intensive care for babies has evolved over time.
Progress: All follow-up for this cohort has finished.
VICS 1979-80
Impact: The VICS 1979-80 cohort is where it all started for the team. Since then, results from this cohort have appeared in scientific journals and in the press. The other VICS cohorts have expanded from the ideas and impact of this cohort.
Progress: All follow-up for this cohort has finished.
Research Findings!
See a list of impactful publications and research results from VICS cohorts.
