DECEMBER 2018
Welcome to the 2018 Victorian Infant Collaborative Study newsletter. We hope this finds you all well and looking forward to the holiday season. We have had a busy year with a lot happening at all the centres involved in the VICS studies.
VICS 2016/2017 Cohort
It has been a big year for VICS this year, with both our 1991/1992 cohort and our newest additions the 2016/2017 cohort, being seen. Our 2016/17 cohort assessments began in July of this year, and we are so delighted to see our newest babies coming back to us as very busy 2 year olds.
All 3 VICS centres- Royal Women’s Hospital, Mercy Hospital for Women and Monash Medical Centre are currently s
eeing our 2 year old participants.
A big thankyou to the families who have participated thus far. The general consensus is that the children enjoy their time with us and parents are very interested in how their children are progressing.
Just a reminder that approximately 50% of the children in VICS are born preterm whilst the other 50% are born at full term. The research team greatly appreciate the time our participating families give us.
An extra big thankyou to our full term born participants (controls). Our study is reliant on the input from our control ch
ildren as well as our preterm infant families, our research simply does not work without it. We are very grateful for the time you give to us. We hope that your time spent with us is rewarding.
Photos of Austin and his mum Emily. Austin is one of our control children, and he had a great day with us! Austin is showing us how well he can climb stairs and jump (gross motor skills)- great job. Thank you to Austin.
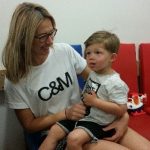


At the 2 year appointment, our team of experienced psychologists and paediatricians assess the children as to their thinking, speaking, fine motor ( drawing, picking small things up)and gross motor skills ( running, jumping) as well as a full general health check.
All parents receive a full report after the visit as to their child’s progress.
Please see some photos below of Chester, Eli and Theodore (some of our preterm born participants) enjoying their Bayley testing with our very experienced psychologist Elaine.




We will be continuing to contact families well into next year, so if you have changed any of your contact details, please let us know.
There may be opportunities for our families to participate again in the future, as this is a study that hopes to understand many aspects of how the children grow up. We try very hard to keep contact details current, if any at any time there are changes, please let us know.
For families of our 1997 and 2005 cohorts, we hope to see you again sometime soon, we will keep you posted.
Emma’s Story
On the 20th May 2016, I went into spontaneous labour with my twins at 27 weeks. I was rushed to St John of God Hospital in Geelong where my boys Eli & Chester entered the world in a hurry. They were held up in front of me then whisked away to be ventilated, wrapped in “Glad” lunch bags and hooked up to tubes and wires. An hour later, I was able to hold my boys’ hands for a few short minutes before they were loaded into a NETS unit & were on the highway up to the NICU at the Royal Women’s Hospital in Melbourne. That night, I remained at St John of God Hospital and had a sleepless night as I was frightened for my two little men. At this point, I didn’t know if I’d see them again.
The following day I was allowed “day release” and travelled the first of many days up the highway to see my boys at the Royal Women’s. I was terribly afraid of what I was going to see & I had no indication if my boys would survive. When I arrived, my boys were still covered with tubes and wires and were sleeping in humidicribs. Again, I was only able to touch their hands but to me that felt amazing. I was advised that my boys would need significant medical attention and to be prepared for the long haul of ups & downs.
From that day onwards, I felt so supported. The nursing staff, carers and doctors made me feel as though I was an extension of my boys and involved me every step of the way. I made it my duty as their mother to learn all of the medical terminology and ensure I understood what was happening so I could make informed decisions.
One day, not long after my boys were born, I was having lunch in the NICU’s family tea room and saw a brochure on the wall calling for participants in the Victorian Infant Collaborative Study. This appealed to me as it would give me further insight into the treatment my boys were receiving which was based upon 26+ years of research in to preterm infants. It also meant that my boys would partake in current research to assist treatments for babies born in the future. I wanted to give back to show that I was so very grateful for those that had come before me and how their participation in the study was helping my boys.
Making contact with VICS was easy and so began a lovely relationship with a team of researchers who are dedicated to not only their study and the health and development of preterm infants, but have a genuine interest in my boys! Whilst we were in the NICU, the researchers regularly visited us at our cots and they explained how their past research has shown improved results which were now common practise across all NICUs. Practises such as snuggling the babies in little nests and giving the babies caffeine have both been as a result of VICS research.
After 59 days, my boys left the Royal Women’s NICU and were transferred to the Special Care Unit at St John of God in Geelong. And after a further 23 days, my boys were discharged home with me with mild chronic lung disease and ongoing fluid on their ears causing low level deafness and chronic ear infections. We were linked in with a great team of doctors & specialists to assist our development. My contact with VICS continued via the Baby Moves App and emails where I would brag about how well my boys were doing post-hospital.
And at 2 years corrected, my boys and I returned to the Royal Women’s for a follow-up appointment. I was terribly anxious driving into the Royal Women’s as the last time I had been there my boys were so fragile and in the NICU. However, this time they were boisterous, adventurous toddlers & I wanted to show the VICS team how well they were doing. We were warmly welcomed and briefed about what the testing would involve. Despite my reservations that we were still behind in language, learning and development the next several hours of “games” & easy questioning revealed that I have two very clever little boys. I drove away from the follow-up feeling that despite their ongoing medical issues, everything I had done to help my boys develop, explore, live and learn was working. My initial concerns were unfounded and I am able to feel proud that my boys are growing into healthy little adventurers.
I am grateful to the VICS team as their genuine interest in their infants & follow-up participants is fostering proven results which will continue to have a profound impact on pre-term babies born in Australia.
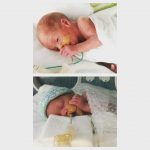

Chester and Eli as newborn infants and again as very happy 2 year olds with mum and nanna.
VICS 91-92 Cohort
We have recently completed assessments for our Victorian Infant Collaborative Study ( VICS) young adult study (91-92 cohort). As part of the study we invited young adults (25 year olds) who were either born very preterm (born before 28 weeks of pregnancy/ born weighing less than 1000g) or were term born from 3 major Victorian hospitals – The Royal Women’s Hospital, Monash Medical Centre and Mercy Hospital for Women. These participants have been previously followed at ages two ,five, eight and eighteen years. We are pleased to report that in total we have assessed 297 participants for the study. As part of our recruitment strategy we used social media especially Facebook to help trace participants who were hard to locate or difficult to contact. It proved to be enormously successful in engaging our young adult participants, the majority of whom responded promptly to our invitation to participate in the study.
The entire VICS team is very grateful to all our participants for their contribution towards this important research. We thank you for your time and effort and your willingness to participate in the study. We are especially indebted to all those who travelled from interstate and very generously gave up their time to be part of the study. It was a pleasure to meet all our participants and to hear about their journey so far.
The next important step is collating and examining the results from various health assessments (physical and mental health) and reporting the outcomes to the wider community. We are very hopeful that the results from this study will help us understand better the health challenges faced by young adults born extremely preterm/low birth weight, and in turn improve long term health outcomes and quality of life. Additionally, these results will be important to inform health practitioners when managing and treating young adults born extremely preterm in the future.
Peter and Leigh, some wonderful VICS participants visiting some pre term babies in the nursery at The Royal Women’s Hospital

Thank you to Peter and Leigh and to everyone who has participated.
Aakash’s Story
I am always eager and ready to participate in a premature follow up study, as it helps towards finding results that would benefit those in the situation that I had previously been in. I have been participating in these studies since a young age.
To be able to give back, aid researchers in discovering more on the development of a premature individual and to help such little ones in need is important to me, both from an individual and societal perspective.
I was born at 25 weeks on 19 October 1992 in Australia, which was also the same year that my family had just migrated from Fiji (in February 1992).
It was a very stressful moment in life for my family, given that I was born 3 months early and battling daily just to live, as well as a new environment for them to adapt in. There was doubt by medical staff that I would be able to pull through, let alone live a disability free life or suffer with a slow intellect.
Today I stand tall with a Criminology degree (which I completed at the age of 24) and am now serving as a proud member for the Government (within the Department of Justice and Regulation).
Participating in this VICS study was a long but eventful day. It ranged from different tests, including my least favourite- blood tests (not a big fan of needles) & also the 24 blood pressure machine, which can be a bit of a hindrance to live with.
I went along with my mum (as a throwback to my childhood appointments) which was also fun.
The staff were nice and attentive. Thank you to everyone for giving a warm reception.
All in all, it was a good day with lifelong memories made.
Thank you for reading and reliving a part of my journey,

Akaash Kumar
Recent publications from the VICS team
Recent publications from the VICS team
First days predict long-term health of preterm babies
New research will allow doctors to more accurately inform and update parents of extremely preterm babies about their baby’s long-term survival and health risks.
The study in 751 babies found that the likelihood of extremely preterm babies surviving and doing so without long-term disability dramatically improved with each day they survived, with the most dramatic improvement happening in the first week after birth.
Babies born before 28 weeks cannot survive without intensive care. Even with intensive care treatment, those born at 23 weeks have only a 45 per cent chance of surviving but those odds dramatically improve if they survive the first week of life and by the time they go home their risk drops to below 1 per cent.
Those who do survive are at higher risk of major long-term disability such as major problems with thinking, walking, talking, hearing, or seeing compared with children born at term (between 37-42 weeks).
The research, published today in the prestigious The Lancet Child and Adolescent Health journal, found that most babies born before 28 weeks will survive if they are offered intensive care, and that 83% who do survive and go home will subsequently have no major long-term disability – compared with 97% of children born on time.
Neonatologist and lead researcher A/Prof Jeanie Cheong, from the Royal Women’s Hospital, Murdoch Children’s Research Institute and University of Melbourne, said the new information was positive news for families of extremely preterm babies.
“Our research has found that a baby’s risk of death dramatically declined in the first few days after birth, and by the time of their discharge home their risk of death was similar to healthy full-term babies. This is very encouraging news for parents who are often very frightened when taking their newborn baby home from hospital,” A/Prof Cheong said.
“Parents are often counselled about their baby’s risk of death and disability before their baby is born, when the mother presents at hospital with impending preterm birth,” A/Prof Cheong said.
“However, we have not been able to accurately update these families on how their individual baby’s risk changes over the course of their intensive care treatment. Parents may be taking home their baby fearing that they are at a much higher risk of death or long-term disability than is the reality,” she said. “Our previous research has shown that depression and anxiety in parents of extremely preterm babies are up to five times higher than the already high rate in parents of children born at term, and the concerns about higher risk of death or long-term disability may be contributing to their worries.
“Now we can tailor the risk information and bring much needed reassurance to parents.”
Lisa’s (2005 VICS cohort) twin boys were involved in the research after Noah and Oliver were born at just 24 weeks gestation. Noah survived just one day.
“I was told all the risks they were to face before they were born, it was very frightening. After losing Noah, I was terrified that Oliver would die even after he was well enough to come home,” Lisa said. “For four years I had a monitor attached to his bed so I wouldn’t have to worry about whether he was breathing or not. I was incredibly anxious.”
Oliver is now a healthy 13 year old with no long-term disabilities.
“It is great that other parents in similar situations can now be reassured by this research and feel more confident when they take home their baby,” Ms Santalusia said.
The highest risk of death or disability were in babies born at the earliest gestations. For babies born at 23 weeks, the chance of survival was around 45 per cent for those offered intensive care, with only 30 per cent predicted to survive without a severe disability.
However, for those babies that did survive, these risks changed dramatically with each day of life. By the time of discharge from hospital, the risk of death decreased to less than 1 per cent, and their chance of surviving free of major disability rose to 70 per cent.
Researchers were able to identify four clinical events that were associated with a higher risk of long-term disability in very extremely preterm babies. They included two that relate to major brain injury (diagnosed by ultrasound of the brain after birth), the baby receiving corticosteroids after birth to treat or prevent lung injury, and needing surgery in the newborn period. Almost one-half of the extremely preterm babies avoided all of these complications, and of those that do avoid those events – 93 per cent survived without a major disability.
The research is part of one of the world’s longest studies into the long-term effects of extremely preterm birth, the Victorian Infant Collaborative Study (VICS), a collaborative group from the four major neonatal hospitals in Melbourne (The Royal Women’s Hospital, Mercy Hospital for Women, Monash Medical Centre and The Royal Children’s Hospital). Every child born before 28 weeks or weighing less than 1000g and born in 1991/92, 1997, 2005 and 2016/17 were invited to take part of the VICS studies.
A Lovely quote from the sibling (Andrew) of one of our VICS 1991/92 Cohort
I am a third year MD student currently at the Royal Women’s Hospital, and I would like to thank you and the other researchers involved for the research recently published in the Lancet, as well as for all the long-term research and push for excellence in neonatal care across the RWH and at Monash Medical Centre.
For my family and myself personally, the value of this research is huge. My twin brother was a part of the ‘91 VICS cohort (born at 28 weeks, and I was just over the 1000g threshold), and both my parents agree that the uncertainty around our prospects was a massive source of anxiety for them. For my family to know that our experience helped create this data behind a collective set of factors that help predict long term disability and conversely provide reassurance to family of severe prematurity babies is wonderful. For myself, it’s been an incredibly humbling experience to learn about the then-experimental treatment I received at birth, and precisely what the outcome could have been without it, and that has made me appreciate the health of my brother and I all the more.
Grant Success Story
A/Prof Jeanie Cheong has secured a $2.5 million CRE in Newborn Medicine five-year grant for the Women’s Newborn Research Team and its partners. This marks a changing of the guard, following on from two similar grants secured by Prof Lex Doyle over the past 10 years.
The main focus for next five years is on knowledge translation.
In A/Prof Jeanie Cheong’s own words “it is about taking the knowledge out to where it really counts and delivering change in clinical practice across the world, along with communicating our research knowledge to the community.”

A/Professor Jeanie Cheong with professor Lex Doyle. Leaders of VICS.
Some other exciting activities to report
Dance PREEMIE- an opportunity for some of our pre term born children in the VICS.
Dance PREEMIE- Dance classes especially designed for children born preterm
Physical activity is such an important way for children to develop their movement skills, keep fit and have fun! Dance PREEMIE is an exciting new intervention that will help children get involved in physical activity as well as improve their movement skills- all through a preschool dance class. What makes Dance PREEMIE unique, is that it is designed especially for children born early or low birthweight (at less than 28 weeks’ gestation or less than 1000g). Dance PREEMIE classes will be taken by teachers who have received extra training from a physiotherapist and will be provided free of charge. We will be trialling Dance PREEMIE in Term 4 2019 and Term 1 2020. At the moment we are asking for expressions of interest from families. This study is brand new, so unfortunately we are only able to offer Dance PREEMIE to children born early/low birthweight at the Royal Women’s Hospital, however we hope to be able to offer the intervention to more children in the future.
Questions about Dance PREEMIE? Please email Kate on kate.cameron@mcri.edu.au
Dance PREEMIE has ethical approval from the Royal Children’s Hospital and is funded by a PRF Seeding Grant.
For the latest physical activity guidelines for children and adults of all ages check out: http://www.health.gov.au/internet/main/publishing.nsf/content/health-pubhlth-strateg-phys-act-guidelines#npa05 or Google: Australia’s Physical Activity and Sedentary Behaviour Guidelines

Kate dancing with Penny.
To update us with your current contact details, including your email address
OR
To find out more about the Victorian Infant Collaborative Study, visit our website:
https://www.vicsinfant-study.org.au/
or find us on Facebook:

